Overview
Scientific Focus
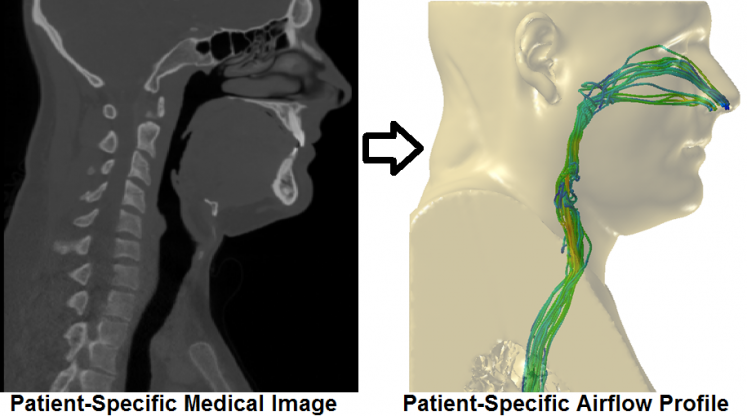
Our laboratory combines computational fluid dynamics (CFD) modeling with three-dimensional (3D) reconstruction to investigate pathophysiology of the ear, nose and throat, as well as the effects of pathologic abnormality on normal functioning of the ear, nose, and throat. Ongoing research projects include:
- Modeling nasal airflow pattern and odorant transport in subjects with normal olfaction and those with sinusitis induced olfactory dysfunction.
- Modeling laryngeal aerodynamic and aeroacoustics patterns in both pathologic and healthy throats.
- Quantification of dorsal and septal deformities in subjects with cleft palate.
- Investigating the role of temporal bone anatomy on conductive hearing loss.
- Modeling flow irrigation in the outer ear to mimic routine testing done for assessing vestibular function.
Selected Achievements
We identified three distinct normal variations in the human nasal vestibule morphology that have not been previously described, namely, Notched, Standard, and Elongated. These distinct morphologies were found across subjects with normal nasal anatomy, as well as subjects with nasal diseases. The nasal vestibule morphology is classified Notched if there is a prominent indentation at the junction of the nasal ala and sidewall; or Standard if it conforms with the “typical” nasal vestibule configuration with some subjects having a very small notch at the level of the internal nasal valve; or Elongated if the level of the nasal ala is elongated. Our report showed that nasal vestibule morphology has significant effects on anterior nasal airflow resistance, but these effects do not extend toward global resistance. This implies that while variabilities in nasal vestibule may not affect overall (global) sensation of nasal patency in healthy subjects.
Several different clinical objective assessments have been developed to better understand the impact of upper airway disease on patients’ quality of life. However, these objective measures have failed to demonstrate strong associations with patient-reported quality of life. In works conducted by our research group using computational methods, we identified a number of CFD airflow variables that demonstrated strong evidence of correlation (up to r=0.82) with patient-reported outcomes for sinonasal conditions such as chronic rhinosinusitis and nasal airway obstruction.
Advanced Training
We currently have several ongoing research opportunities (see Lab Members) and are looking for highly motivated resident(s) and student(s) with interest in computational modeling of fluid flow in the ear, nose, and throat to join us.
Contact Us
Dennis Onyeka Frank-Ito, Ph.D.
Department of Head and Neck Surgery & Communication Sciences
Duke University Medical Center
Box 3805
Durham, NC 27710
E-mail: dennis.frank@duke.edu
Phone: (919) 681-7247
Fax: (919) 613-6524
Latest Publications
Funded Projects
Grants
Publications
Lab Members
Faculty Members
- David L. Witsell, MD, MHS
- Debara L. Tucci, MD, MBA, MS
- Jeffrey R. Marcus, MD
- Wilkins Aquino, PhD
- Eileen M. Raynor, MD
- David W. Jang, MD
- Rose J. Eapen, MD
- David M. Kaylie, MD, MS
- Charles R. Woodard, MD
Residents
Current: Open Position
Former: Chad Whited, MD; Jarrod Keeler, MD; Aniruddha Patki, MD; Mirabelle Sajisevi, MD; Kevin J. Choi, MD
Students
Current: David Carpenter; John Lu
Former: Jiadong Yin; Vaib Ramprasad; Jennifer Zou